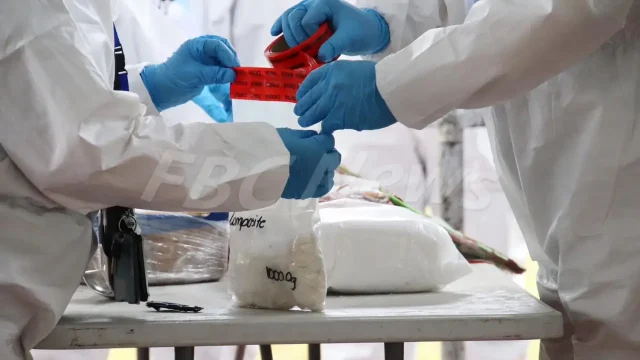
[Photo: FILE]
While the Needle Syringe Program is regarded as one of the most effective ways of minimizing the spread of HIV infections, it is a sensitive approach and may trigger public resistance.
Jason Mitchell, the HIV Advisor for Australia’s Department of Foreign Affairs and Trade, says that the HIV-AIDS Act 2011 allows the government to introduce the Needle and Syringe Program, but there are other elements that need to be considered.
Mitchell says that in the past, any public health intervention introduced in Fiji and other countries met with significant resistance from communities.
“Good examples that we all have experience with are condoms and family planning. When we first introduced those to Fiji and in many other countries, it was the same experience. People immediately said, “You are promoting promiscuous sex, you’re going to make people have early sex, all these sorts of things. And what we respond to them was, we are responding to public health needs.”
However, Mitchell stresses that the Needle and Syringe Program is a public health measure and a harm reduction approach to reducing HIV infections.
“Drugs are here, and we don’t know what measures will be put in place by our government and other authorities to remove drugs as an issue in this country. In the meantime, we have this issue of HIV and hepatitis C impacting people who are utilizing drugs through unsafe practices. And the intervention for that is to introduce a needle and syringe program along with an effective peer education program, which is already underway, and it’s quite successful.”
Mitchell explains that by providing drug users with sterile needles and syringes, they will stop sharing them.
He adds that clinical data show many people who are infected are from the same family groups.
“In Fiji, which is unique compared to other countries, we inject in groups, like we share food in groups, we share cover, one bowl we share with a group, alcohol, we talk about alcohol, one glass, we are sharing needles and syringes in that way. So people are becoming infected in groups.”
Mitchell further states that if Fiji does not have an effective Needle and Syringe Program and a condom program, the country will continue to see new HIV infections.
Fiji recorded over 2,000 new HIV cases last year, compared to 1,583 in 2024 – an increase of 26 percent.
Experts warn that Fiji could record more than 2,000 new HIV infections again this year if urgent action is not taken to address the escalating crisis.

 Yvonne Ravula
Yvonne Ravula