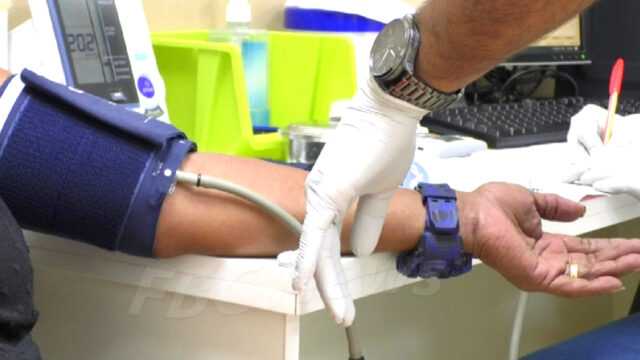
Fiji’s Public Health Act 1935 is no longer fit for purpose as the country grapples with rising non-communicable diseases, repeated disease outbreaks and growing climate-driven health risks.
Health Minister Dr Atonio Lalabalavu told Parliament these pressures have made sweeping reforms necessary to modernise and strengthen the public health system.
The Minister said that the existing law had remained largely unchanged for nearly 90 years and was designed for a colonial-era health system that no longer reflects modern Fiji.
He said the country now faces a very different burden of disease, with non-communicable diseases accounting for about 70 per cent of deaths, alongside increasing risks from dengue, leptospirosis, water contamination and emerging infections.
The Public Health (Amendment) Bill 2026 was passed after extensive debate that centred on the balance between stronger state powers and protections for citizens.
The reforms expand inspection and enforcement authority, modernise disease surveillance systems, and strengthen outbreak response mechanisms across divisions and rural areas.
Dr Lalabalavu said the Bill was shaped by lessons from COVID-19, which exposed gaps in quarantine powers, emergency response coordination and disease notification systems.
The new framework strengthens surveillance, formalises outbreak teams and gives environmental health officers broader operational authority during health emergencies.
He said the legislation also modernises governance by restructuring the Central Board of Health to include medical, engineering, legal and local government expertise. The aim, he said, is to improve oversight and ensure decisions reflect technical and multidisciplinary input.
A major shift under the Bill is the expansion of rural and local authority functions in public health enforcement.
Government said this would bring services closer to remote communities in Kadavu, Rotuma, Lau and Lomaiviti, where access to inspections, sanitation oversight and compliance enforcement has been limited.
The Bill also strengthens regulation of water quality, sanitation systems, waste management and housing standards. Government said these changes are critical for disease prevention, especially in informal settlements and fast-growing urban areas where infrastructure pressure is increasing.
Another key reform is the overhaul of penalties. Fines that previously ranged from as low as $2 to $40 have been replaced with significantly higher penalties designed to act as a deterrent against public health breaches.
However, Opposition MP Premila Kumar raised concerns over the breadth of new enforcement powers. She warned that provisions allowing health officers to enter homes, issue orders and enforce isolation measures needed clearer safeguards and appeal mechanisms.
She also questioned the use of broad terms such as nuisance and insanitary condition, saying they could lead to inconsistent enforcement and unfair targeting of vulnerable communities, including informal settlers and small street vendors.
Kumar further raised concerns about limited resourcing for rural local authorities and environmental health services. She said current funding is heavily weighted towards salaries, leaving little for operational needs such as transport, equipment and field inspections.
Opposition MP Jone Usamate supported the intent of the Bill, saying it aligns legal powers with current health policy needs. He said COVID-19 highlighted the importance of rapid response powers, especially in outbreak control and quarantine enforcement.
However, he also cautioned that expanded authority must be matched with accountability, adequate funding and public awareness to ensure effective implementation across all communities.
In response, Dr Lalabalavu said environmental health officers are already deployed nationwide, including remote islands and will play a central role in implementing the new framework.

 Litia Cava
Litia Cava